Introduction to Root Canal Therapy
Root canal therapy, also known as endodontic treatment, is a vital procedure in dental care designed to save a severely damaged or infected tooth. When the pulp—the soft tissue inside the tooth containing nerves and blood vessels—becomes inflamed or infected due to deep decay, trauma, or repeated dental procedures, a root canal is necessary to remove the affected tissue. This treatment not only alleviates pain but also preserves the natural tooth, maintaining the integrity of the dental arch and overall oral health.
Despite common misconceptions, root canal therapy is not as painful as often portrayed. Advancements in dental technology and anesthesia have made the procedure relatively pain-free and highly effective. Modern endodontic techniques ensure that patients experience minimal discomfort during and after the treatment, making root canals a routine and reliable option for tooth preservation.
Anatomy of the Tooth and the Role of the Pulp
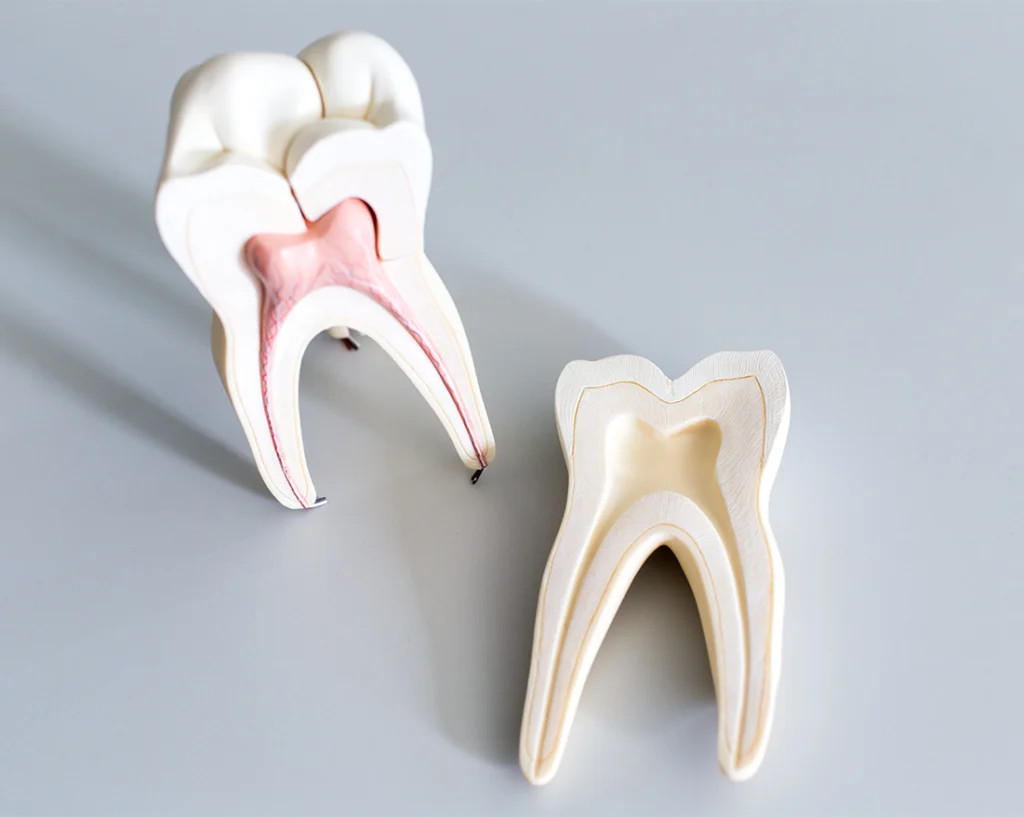
Understanding the anatomy of a tooth is essential to comprehend the necessity and function of root canal therapy. A tooth is composed of several layers:
Enamel
The enamel is the hard, outermost layer of the tooth, serving as the primary barrier against physical and chemical damage. It is the hardest substance in the human body, protecting the underlying structures from decay and wear.
Dentin
Beneath the enamel lies the dentin, a softer layer containing microscopic tubules that connect to the pulp. Dentin provides additional strength to the tooth and plays a role in sensation, transmitting pain signals when the tooth is damaged or decayed.
Pulp
The pulp is the soft tissue located at the center of the tooth, encompassing nerves, blood vessels, and connective tissue. It is crucial during tooth development, providing nutrients and sensory functions. However, once the tooth is fully mature, the pulp becomes less necessary, and its health is vital for maintaining the tooth’s integrity.
Damage or infection to the pulp can lead to severe pain, sensitivity, and the potential spread of infection. Root canal therapy addresses these issues by removing the compromised pulp, cleaning and disinfecting the canals, and sealing the tooth to prevent future infections.
Signs and Symptoms Indicating the Need for a Root Canal
Recognizing the signs that indicate a need for root canal therapy is crucial for timely intervention and preservation of the tooth. Common symptoms include:
Persistent Tooth Pain or Sensitivity
Continuous pain or sensitivity to hot and cold temperatures is a primary indicator of pulp damage. This discomfort often worsens over time and can become severe if left untreated.
Discomfort When Chewing or Applying Pressure
Experiencing pain while chewing or applying pressure to a specific tooth suggests that the pulp may be compromised, requiring immediate attention.
Swelling and Tenderness in the Nearby Gums
Localized swelling and tenderness around the affected tooth are signs of infection or abscess formation, necessitating urgent dental care.
Darkening or Discoloration of the Tooth
A noticeable change in the color of a tooth, turning darker or grayish, can indicate pulp necrosis (death) and the need for a root canal.
Presence of a Pimple-like Bump on the Gums
A small, pimple-like bump on the gums near the affected tooth may signal the formation of an abscess, a pocket of pus caused by infection.
These symptoms suggest irreversible damage to the pulp and the presence of infection, making root canal therapy essential to alleviate pain and prevent further complications.
Causes of Pulp Damage or Infection
Several factors can lead to damage or infection of the pulp, necessitating a root canal:
Deep Decay (Cavities)
Untreated cavities allow bacteria to penetrate deep into the tooth, reaching the pulp and causing infection. This bacterial activity leads to inflammation and pain, ultimately requiring endodontic intervention.
Cracked or Fractured Teeth
Trauma to the tooth, even if not visibly apparent, can create pathways for bacteria to invade the pulp chamber. Cracks can also expose the pulp to external irritants, leading to infection and pain.
Repeated Dental Procedures
Multiple restorations or fillings on the same tooth can weaken the tooth structure, increasing the risk of pulp irritation and infection. Over time, this can compromise the health of the pulp, necessitating a root canal.
Trauma
Physical injuries, such as a blow to the mouth, can damage the pulp even if the outer tooth remains intact. This trauma can lead to pulp necrosis and the need for endodontic treatment.
Addressing these causes promptly is essential to prevent the progression of pulp damage and avoid more invasive treatments or tooth loss.
The Science Behind Root Canal Treatment
Root canal therapy is a meticulously structured procedure aimed at removing infected or damaged pulp, disinfecting the tooth’s interior, and sealing it to prevent further infection. Here’s a detailed look at the steps involved:
Diagnosis and Imaging
The initial phase involves diagnosing the extent of pulp damage or infection. Dentists utilize X-rays or Cone Beam Computed Tomography (CBCT) scans to assess the tooth structure, root anatomy, and the presence of any abscesses or fractures. Accurate imaging is crucial for effective treatment planning.
Local Anesthesia
To ensure patient comfort, local anesthesia is administered to numb the affected area. This makes the procedure virtually painless, allowing the dentist to perform the treatment without causing discomfort.
Accessing the Pulp Chamber
The dentist drills a small opening in the crown of the tooth to reach the pulp chamber. This access point allows for the removal of the infected or damaged pulp and the subsequent cleaning of the canals.
Removing the Pulp
Specialized endodontic tools are used to extract the pulp from the canals. The canals are then thoroughly cleaned and disinfected to eliminate bacteria and prevent reinfection.
Shaping and Disinfecting the Canals
The canals are shaped to accommodate the filling material, typically gutta-percha. Antiseptic and antibacterial solutions are used to ensure all traces of infection are removed, providing a clean environment for the filling.
Filling the Canals
Once the canals are cleaned and shaped, they are filled with a biocompatible material called gutta-percha. This material seals the canals, preventing bacteria from re-entering and causing further infection.
Restoring the Tooth
After the root canal is complete, the access hole is sealed with a temporary or permanent filling. Depending on the extent of the damage, a dental crown is often placed over the tooth to restore its strength and appearance, ensuring it can function effectively without breaking.
Pain Management and Recovery After a Root Canal
One of the most significant concerns patients have about root canal therapy is pain management. Modern advancements have made root canals relatively pain-free and manageable, both during and after the procedure.
Pain During the Procedure
With the use of local anesthesia, patients typically do not feel pain during the root canal procedure. Any discomfort experienced is usually minimal and comparable to that of routine dental treatments like fillings.
Recovery Process
Post-treatment recovery is generally straightforward. Patients may experience mild discomfort or sensitivity for a few days following the procedure, which can be managed with over-the-counter pain medications such as ibuprofen or acetaminophen.
Managing Discomfort
To alleviate any post-procedure discomfort, patients can:
- Take Pain Relief Medications: Ibuprofen or acetaminophen can help reduce inflammation and control pain.
- Avoid Hard or Chewy Foods: Protect the treated tooth by avoiding foods that require excessive chewing until the final restoration is placed.
- Use Ice Packs: Applying a cold compress to the outside of the mouth can help reduce swelling and numb pain.
Follow-up Appointments
Follow-up visits are essential to ensure proper healing and the placement of the final restoration, such as a dental crown. These appointments allow the dentist to monitor the treated tooth and address any concerns that may arise.
Restoration and the Role of Dental Crowns
After a root canal, restoring the tooth’s functionality and appearance is crucial. Dental crowns play a significant role in this restoration process.
Importance of Dental Crowns
Root canal-treated teeth often become more brittle and prone to fractures due to the removal of the pulp and loss of structural integrity. A dental crown provides the necessary strength and protection to prevent the tooth from breaking and to restore its natural appearance.
Process of Crown Placement
The crown placement process involves several steps:
- Preparation: The dentist reduces the size and shape of the treated tooth to accommodate the crown.
- Impressions or Digital Scans: Precise molds or digital scans of the tooth are taken to create a custom-made crown that fits perfectly.
- Fitting the Crown: Once the crown is ready, it is cemented onto the prepared tooth, restoring its appearance, strength, and functionality.
With proper care, a dental crown can last many years, ensuring the longevity of the root canal-treated tooth.
When a Root Canal is Not Enough
While root canal therapy is highly effective, there are instances where it may not be sufficient to save the tooth:
Inadequate Cleaning of the Canals
If the canals are not thoroughly cleaned, bacteria can remain, leading to reinfection and the need for retreatment.
Complicated Anatomy
Teeth with curved or narrow canals can harbor bacteria even after treatment, increasing the risk of failure. Specialized techniques and tools are required to address these complexities effectively.
Delayed Treatment
Delays in addressing pulp damage or infection can result in widespread infection and significant deterioration of the tooth structure, making root canal therapy insufficient. In such cases, additional surgical options like apicoectomy (removal of the root tip) may be necessary.
When root canal therapy fails, retreatment or extraction may be required to resolve the issue and prevent further complications.
Alternatives to Root Canal Therapy
While root canal therapy is the preferred method for saving a damaged or infected tooth, there are alternative treatment options, primarily tooth extraction.
Tooth Extraction
Extraction involves removing the affected tooth entirely. While this can resolve the immediate pain and infection, it has several drawbacks:
- Loss of Natural Tooth: Removing the tooth disrupts the dental arch and can lead to shifting of surrounding teeth.
- Need for Replacement: Replacing an extracted tooth often requires implants, bridges, or dentures, which can be more costly and complex compared to saving the tooth with a root canal.
Comparison of Root Canal Therapy and Extraction
| Aspect | Root Canal Therapy | Tooth Extraction |
|---|---|---|
| Preservation of Natural Tooth | Yes | No |
| Functionality | Restores full functionality | May require prosthetics |
| Aesthetics | Maintains natural appearance | May affect smile and facial structure |
| Cost | Generally lower than implants or bridges | Requires additional treatments for replacement |
| Procedure Complexity | Requires specialized treatment | Simple extraction, but replacement is complex |
In most cases, root canal therapy is the preferred option as it preserves the natural tooth, maintains the integrity of the dental arch, and avoids the need for additional procedures required by tooth extraction.
Prevention and Long-term Care for Root Canal-Treated Teeth
Preventing the need for root canals is the best approach to maintaining oral health. However, for those who have undergone the procedure, proper care is essential to ensure the longevity of the treated tooth.
Preventive Measures
Maintaining excellent oral hygiene can prevent the development of conditions that lead to root canals:
- Regular Brushing and Flossing: Brush twice a day with fluoride toothpaste and floss daily to remove plaque and prevent cavities.
- Routine Dental Check-ups: Visit the dentist every six months for cleanings and examinations to catch and treat issues early.
- Healthy Diet: Limit sugary and acidic foods that contribute to tooth decay and enamel erosion.
- Use of Fluoride: Fluoride strengthens tooth enamel and helps prevent cavities.
Care for Root Canal-Treated Teeth
Proper care post-root canal ensures the treated tooth remains healthy and functional:
- Follow-up Visits: Attend all scheduled appointments to monitor the healing process and ensure the final restoration is placed correctly.
- Avoid Excessive Force: Refrain from chewing hard or sticky foods on the treated tooth to prevent damage.
- Maintain Oral Hygiene: Continue diligent brushing and flossing, paying special attention to the restored tooth to prevent decay and gum disease.
- Protect with a Crown: Ensure that a dental crown is placed as recommended to provide structural support and protect the tooth from fractures.
With proper maintenance, root canal-treated teeth can last a lifetime, providing the same functionality and appearance as natural teeth.
Addressing Fears and Misconceptions About Root Canals
Root canal therapy is often surrounded by fear and misconceptions, primarily due to outdated portrayals in media and anecdotal accounts. However, modern dentistry has significantly improved the procedure, making it a safe and effective treatment option.
Common Fears
Many patients fear that root canals are extremely painful or dangerous. These fears are largely unfounded due to advancements in dental technology and anesthesia.
Reassuring Facts
- Effective Anesthesia: Local anesthesia ensures that patients do not feel pain during the procedure.
- High Success Rates: Root canals have a high success rate, with most treated teeth lasting a lifetime when properly restored and maintained.
- Minimal Discomfort: Post-procedure discomfort is typically mild and manageable with over-the-counter pain medications.
- Advanced Techniques: The use of digital imaging, rotary instruments, and improved materials has made root canal therapy faster, more precise, and less invasive.
Statistical Evidence
Studies have shown that root canal therapy is a highly successful procedure, with success rates exceeding 90%. When combined with appropriate restorations, treated teeth can function normally for decades.
Patient Experiences
Most patients report that their root canal treatment was no more painful than getting a filling. The relief from persistent tooth pain after the procedure further underscores its effectiveness in resolving dental issues.
Understanding the realities of root canal therapy can help alleviate fears and encourage individuals to seek timely treatment when necessary.
Conclusion
Root canal therapy is a safe, effective, and essential procedure for saving teeth that are severely damaged or infected. By removing the compromised pulp, disinfecting the canals, and restoring the tooth with a crown, root canals preserve the natural tooth structure, maintain oral health, and alleviate pain. Misconceptions about the procedure being overly painful are dispelled by modern advancements in dental technology and anesthesia, making root canals a relatively comfortable experience for patients.
Early intervention is crucial; recognizing the signs and symptoms of pulp damage can prevent the need for more invasive treatments or tooth extraction. Maintaining excellent oral hygiene and regular dental check-ups further reduce the risk of conditions that lead to root canals. For those who have undergone the procedure, proper care ensures the longevity and functionality of the treated tooth.
Investing in root canal therapy not only saves the natural tooth but also contributes to overall oral health and quality of life. Patients are encouraged to seek prompt dental care when experiencing symptoms of tooth pain or infection, ensuring effective treatment and the preservation of their natural smile.